Restrictive policies have been implemented by the governments in order to reduce COVID-19 transmission. However, it is crucial to take into consideration that #StayAtHome directives themselves can have adverse effects, including reduced physical activity and the accompanying consequences. These include not only physical issues but also psychological effects.
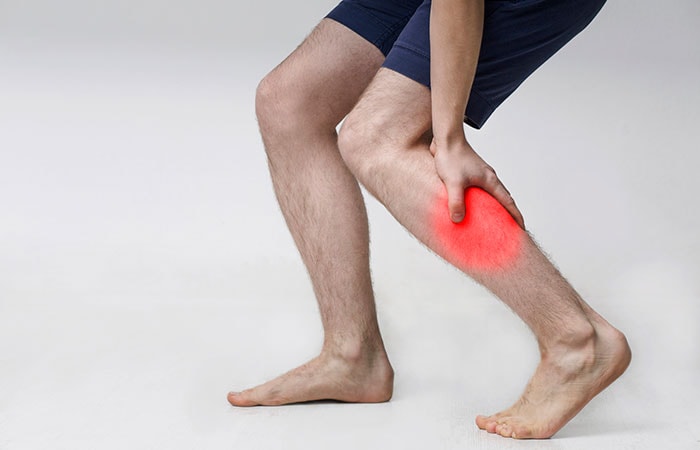
This pandemic has led many of us to long hours sitting in front of a computer table as we work from homes or while you home school your kids. Then we retreat ourselves to the couch to hide from the news only to binge-watch an entire Netflix series without getting up from our seat. A sedentary lifestyle isn’t healthy, and it could put us at an increased risk for developing a blood clot such as a deep vein thrombosis (DVT). Adverse outcomes like DVT can be traced directly to the effects of ‘StayAtHome’ directives.
In a case report published in the Interactive Journal of Medical Research in January 2021, Deep vein thrombosis as a result of Stay-At-Home directives had been reported. The only identified cause of DVT was reduced mobility due to preventive social isolation during the COVID-19 pandemic. Klok et al. have also reported the incidence of thrombotic complications in 184 COVID positives (ICU) patients in the Netherlands. COVID-19 may predispose to both venous and arterial thromboembolism due to immobilization, excessive inflammation, diffuse intravascular coagulation, and hypoxia.
Khan et al. reported that COVID-19 patients are at increased risk of thrombosis for many reasons including immobility, inflammation, and factors contributing to a hypercoagulable state. Based on a retrospective study Karaali (2021) has also reported that COVID-19 confinement seems to be associated with increased rates of DVT. Healy et al. had also provided evidence that computer-related seated immobility and prolonged work; defined as immobility for at least 10 hours within 24 hours and at least 2 hours at a time without getting up is a risk factor for venous thromboembolism that includes both DVT and pulmonary embolism.
What exactly is DVT?
It is the formation of a blood clot in a deep vein, most commonly in the legs or pelvis. When a clot forms inside one of your veins, it won’t always dissolve on its own. DVT can partly or completely block the flow of blood through the vein. The life-threatening concern with DVT is the potential for a clot to embolize, travel as an embolus through the right side of the heart, and become lodged in a pulmonary artery that supplies blood to the lungs. This is pulmonary embolism (PE) which requires immediate medical attention. Many people are unaware they have DVT as it can occur without noticeable symptoms. Those that do experience symptoms may experience pain or cramping in the leg, usually starting at the calf, swelling in the leg, warmth in the affected area, red or blue skin discoloration etc.
Venous thrombosis tends to occur in areas with decreased or mechanically altered blood flow such as the pockets adjacent to valves in the deep veins of the leg. While valves help to promote blood flow through the venous circulation, they are also potential locations for venous stasis and hypoxia. As blood flow slows, oxygen tension declines with a coincident increase in hematocrit. The hypercoagulable micro-environment that ensues may down regulate certain antithrombotic proteins that are preferentially expressed on venous valves including thrombomodulin and endothelial protein C receptor (EPCR). In addition to reducing important anticoagulant proteins, hypoxia drives the expression of certain procoagulants. Among these is P-selectin, an adhesion molecule which attracts immunologic cells containing tissue factor to the endothelium. As the ratio of procoagulants to anticoagulants increases, so does the risk of thrombus formation.
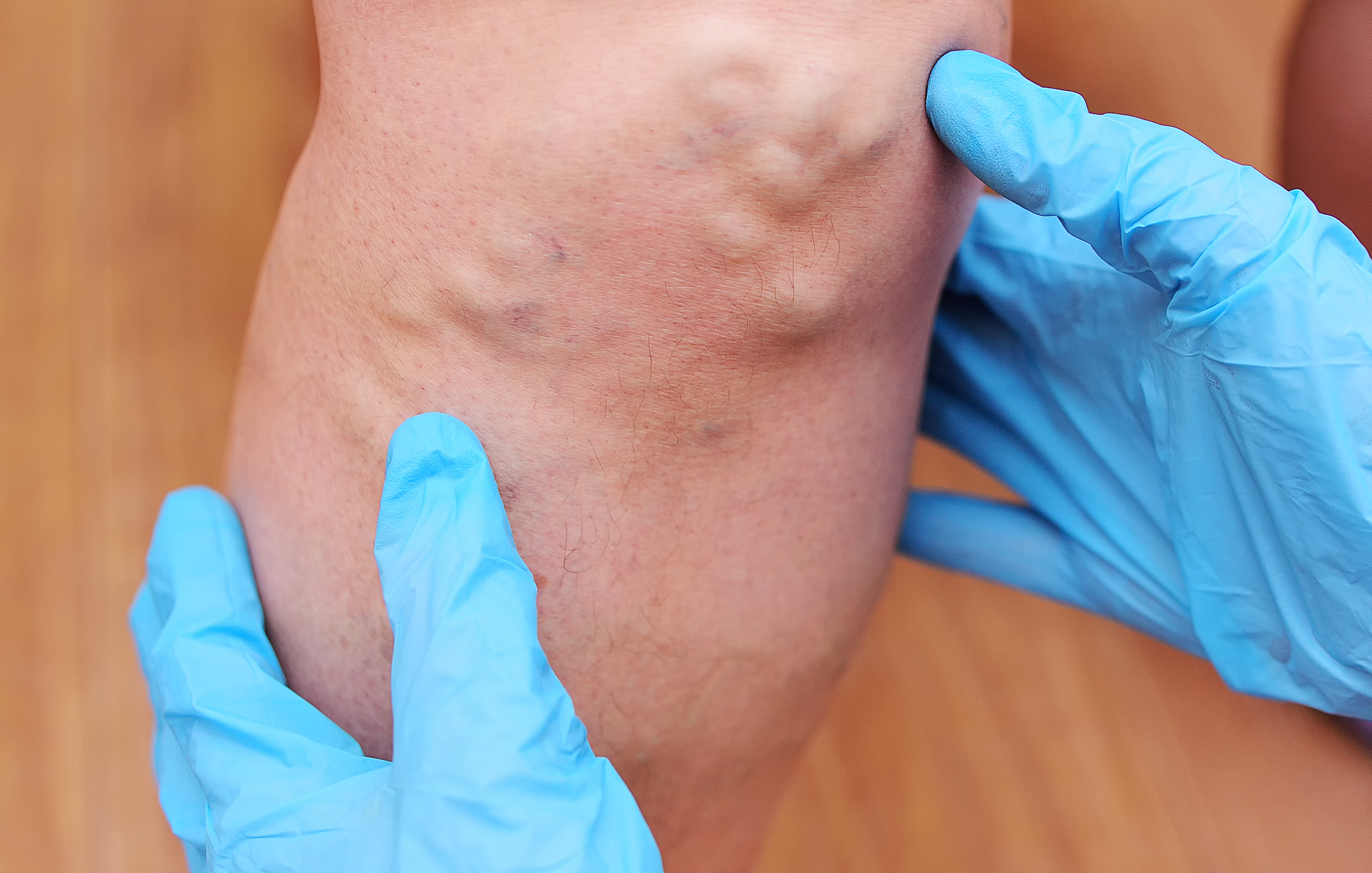
DVT can be caused by anything that prevents your blood from circulating including contraceptives, medications, hormonal therapy, obesity, smoking etc. It may be a surprise to some however, one of the common lifestyle factor that can be responsible is none other than reduced physical activity/physical inactivity. Prolonged sitting can lead to the formation of blood clots in the legs. When you sit for a long period of time, the blood flow to your legs slows down, and when your legs are still and hanging down, blood tends to pool in the muscular beds of the calf. These factors can make it easier for a clot to form and increase your risk for DVT. We’re seeing that during this pandemic time one of the biggest recreational activities is playing video games and binge-watching TV series for hours without a break. This sedentary lifestyle can easily predispose us to DVT.
Clots can also form within an artery. According to a study published in Radiology in 2020, COVID-19 is associated with life-threatening blood clots in the arteries of the legs. Researchers said COVID-19 patients with symptoms of inadequate blood supply to the lower extremities tend to have larger clots and a significantly higher rate of amputation and death than uninfected people with the same condition. During the peak of the COVID-19 pandemic in New York City, radiologists observed an increase in patients testing positive for lower extremity arterial thrombosis on CT angiography exams. In March and April 2020, they identified 16 COVID-19-positive patients for symptoms of leg ischemia. It’s been said that COVID-19’s association with lower extremity arterial thrombosis is likely related to a combination of factors including an increased tendency of the blood to clot, damage to the lining of the arteries, and immune reactions tied to the SARS-CoV-2 virus and COVID-19 infection.
How to Prevent DVT?
Anticoagulants have been suggested for use in COVID-19 to mitigate the risk of venous and arterial thromboembolism. Strict preventive measures such as exercise training, prophylactic drug use, and education about thrombosis risk in people staying at home through the mass media should be considered to prevent immobility-related DVT during the COVID-19 quarantine. Simple lifestyle modifications can also help to reduce the risk. Some simple tips to keep your blood flowing include ankle pumps, leg extension, and seated march, etc. During these times don’t stop your child from playing the games and yourself from watching your favourite Netflix series continuously. Just be aware, enjoy it, and don’t forget to take a break and continue to Stay-At-Home.
Large-scale studies exploring thrombosis in the context of COVID-19 are awaited as this could be an area of intense study in the future.
![]()

A hardworking and tenacious MS Industrial Biotechnology student with a balance of theoretical and practical knowledge. A self-motivated researcher with a strong desire to build a scientific career and aiming at constant professional up-gradation.